Receiving a kidney from a living donor is one of the options you may have. Discover the risks and benefits of receiving a living donor kidney.
Why should I consider getting a living donor kidney?
A transplant from a living donor is the best option for most kidney transplant candidates.
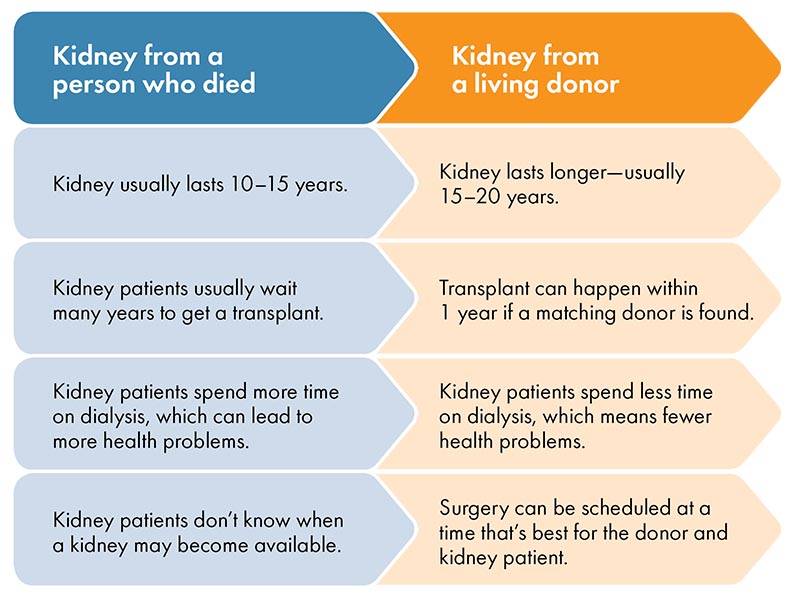
There are many reasons why a kidney from a living donor is better than a kidney from someone who has died:
Who can be a living donor?
Doctors have been doing transplants from living donors for over 50 years, and nationally over 5,000 people donate a kidney every year. Although the restrictions vary from transplant center to center, living donors are typically volunteers who:
- Are 18 years old or older.
- Are healthy and do not have kidney disease.
A living donor may be anyone – from family, friends, or neighbors of the kidney patient to a complete stranger. Donors do not have to be the same race, age, blood type, or sex as the kidney patient.
What tests do donors need for transplant evaluation?
The medical team compares the blood of the donor and kidney patient to see if they are a match.
If they are a match, donors will go through evaluation, a set of medical and psychological tests such as:
- Blood pressure check
- Heart rate and lung function tests
- Blood and urine tests
- A test to help doctors see the blood vessels of the kidney
- Breast exam and Pap smear to test for cervical cancer (for women)
- Colonoscopy to test for colon cancer (for those over age 50)
The purpose of the evaluation is to make sure that the donor is healthy enough to have surgery and the donation is likely to work.
The donor can get all of these tests at a time that fits with their schedule, without having to stay overnight in the hospital. Donors also talk to a social worker or counselor who makes sure they have a support system, such as family and friends who can help them after the transplant.
How long does the evaluation process take?
The donor’s evaluation may take several months, depending on the health of the donor and how quickly they can do the tests.
How can living donors donate a kidney?
There are many ways to donate a kidney.
- Directed donation: A living donor donates a kidney to a specific kidney patient.
- Non-directed donation: A living donor donates a kidney to someone they don’t know. The living donor may do this for personal or spiritual reasons.
What if I have a donor, but they aren’t a match or a great match?
Sometimes a donor isn’t a good match for the specific kidney patient they want to donate to.
Even so, they can still help the patient they know get a living donor transplant.
An exchange program, called a paired donation or a donor chain, makes it possible for 1 donor to help more than 1 kidney patient:
- Paired donation: A paired donation takes place when 2 kidney patients have donors who aren’t good matches for them. The 2 patients swap donors so each can get a kidney that’s a good match for them.
- Donor chain: A chain helps a group of kidney patients who have donors who are healthy but aren’t matches. Swapping donors helps the whole group, or chain, of kidney patients. Sometimes 20 or more kidney patients in a chain are able to get living donor transplants!
Desensitization can help if a kidney patient has extra antibodies, which will attack almost any transplanted kidney – this happens in 1 in 3 patients.
Antibodies are proteins in your blood that help your body fight disease. This can make it very hard or impossible to get a kidney transplant from a donor. In desensitization, you get a blood treatment that takes out your antibodies and replaces them with new ones. The treatment is similar to hemodialysis.
Your body will make new antibodies over time, and these new antibodies are less likely to attack a donor kidney. You may also get medicine to stop the unwanted antibodies from coming back.
You may need treatments both before and after your transplant. It may take several weeks of treatments before you’re ready for a transplant, or you may be ready after just 1 treatment. It only lasts for a short time, so usually you can only use this procedure if you have a living donor.
Desensitization may not be available in all transplant centers and it can be very costly. Talk to your healthcare team about if this is an option for you or if they can recommend a center that offers this treatment.
What are the risks to living donors?
There are risks to all surgeries. There are medical, emotional, and financial risks to a kidney transplant. The transplant team keeps living donors as safe as possible. They will not let someone donate if they face any large risks. A Living Donor Advocate is a social worker, nurse, or doctor who protects the rights and health of living donors.
What are the medical risks of donor surgery?
Normally, doctors remove the kidney through an opening only a few inches long. If there are problems, the opening may have to be larger and recovery time takes longer.
Donors may have some short-term problems from surgery, such as:
- Bloating
- Feeling sick to their stomach
- Scars and pain
- Feeling tired and weak
More serious problems from surgery happen in less than 5% of donors (less than 1 in 20 donors).
The surgical team does everything they can to avoid these problems. These could include:
- Problems from being put to sleep, such as confusion, pneumonia, stroke, or heart attack
- Infection
- Fever
- Bleeding and blood clots
The risk of death is less than 3 in 10,000 donors – this is much less than 1% of donors.
Can living donors still have children after they donate?
Yes, both men and women can donate and still have children. Women should wait 1 year after donating before getting pregnant so that their bodies can heal fully.
What are the financial risks of living donation?
Medicare or the kidney patient’s private insurance will cover the donor’s medical costs. However, most insurance companies don’t cover:
- Time off from work and childcare
- Meals
- Parking and gas
- Hotel costs during testing, surgery, and recovery
Donation can sometimes change the donor’s ability to get or afford health, disability, or life insurance. Donors may also have issues getting work in military service, law enforcement, aviation, and fire departments.
What other risks are there for living donors?
The donor may feel upset or guilty if the kidney they donated isn’t working well. The donor’s relationship with the kidney patient might become strained if the kidney ever stops working.
There’s no way to know for sure how long the donor kidney will work. A living donor kidney usually lasts 15–20 years, but it may only work for a few years or not work at all.
What if the donor wants to stop the process?
A person who’s being tested as a living donor can change their mind about donating at any point, for any reason – even on the day of the surgery. There is no penalty for wanting to stop. The transplant team cannot tell the kidney patient anything about the donor unless the donor agrees.
Will a living donor have health problems after donating?
Most living donors who follow a healthy lifestyle after surgery remain just as healthy after donation as people who have not donated. For most donors, the remaining kidney works fine for the rest of their life.
Most studies on the long-term outcomes of donors have followed donors for only the last 20 years.
For this reason, there is little information about the 40–50 year outcomes for donors.
Some kidney donors get high blood pressure or diabetes, which doctors can treat with medicine. People who donate a kidney have a very small chance of developing kidney disease. If it does happen, the donor is put at the top of the deceased donor waiting list to get a kidney transplant.
Women should talk with the transplant team about a small risk of high blood pressure during any future pregnancies.
What is the donor surgery like?
The donor and kidney patient are admitted to the hospital on the morning of the surgery. Both surgeries happen at the same time and take 3–5 hours.
There are 2 main types of surgery:
Laparoscopy: This procedure uses a wand-like camera placed in small cuts in the donor’s belly.
It lets doctors view the kidney and take it out through a small cut. Doctors will then stitch the cuts closed.
The benefits of this type of surgery include:
- Shorter hospital stay
- Shorter recovery time
- Smaller cuts
- Fewer problems after surgery
Open surgery: Doctors cut open the donor’s belly to take out the kidney. Then they close the cut with stitches.
What happens to the donor’s kidney function during and after surgery?
At the time of donation, the living donor will lose half of their kidney function. However, within 3-6 months, the remaining kidney is able to provide 70% of their initial kidney function. For most people, this is more than they need for the rest of their life.
What is recovery like after donation and how long does it take?
Donors usually feel the most pain the first week after surgery, and can take medicine for their pain. Many donors say that seeing the kidney patient start to feel better helps them forget about their own pain.
Donors usually stay in the hospital for 1–2 days. After leaving the hospital, donors have to rest at home, usually for about a week, while their body begins to heal. Over time, they start to feel better and are able to do more. Most donors can drive and return to their normal lives in 4 weeks.
How does the donor have to care for their health after donating?
Transplant centers follow up with donors for at least 2 years after donation to make sure that they’re healing well and are healthy. After they’ve recovered, donors return to the care of their regular doctor.
They should have their blood pressure and kidney function checked regularly for the rest of their lives.